NEWSROOM
-
Sensory Neurons Help Tumors Evade Immunotherapy in Triple-Negative Breast Cancer
On February 6, 2026, researchers from Fudan University Shanghai Cancer Center published a study in Cell titled “Sensory neurons drive immune exclusion by stimulating a dense extracellular matrix in the breast cancer tumor microenvironment”. The study was led by Prof. Zhi-Ming Shao, Director of the Breast Cancer Medical Center, and Prof. Yi-Zhou Jiang, Vice, Director of the hospital, in collaboration with Prof. Jinfei Ni from the Institute for Translational Brain Research at Fudan University. The team reported that tumor-infiltrating sensory neurons can drive resistance to immunotherapy in triple-negative breast cancer (TNBC). Using multiple animal models, the team further demonstrated that a migraine drug can enhance the effectiveness of immunotherapy, suggesting a potential strategy to overcome treatment resistance.
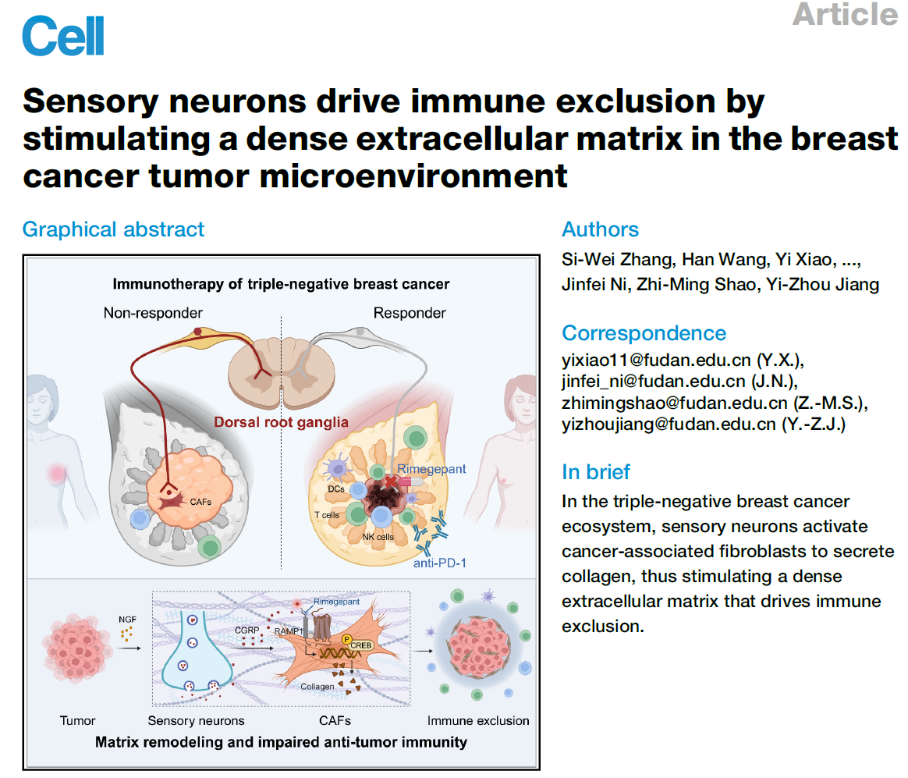
Figure 1. Targeting sensory neurons overcomes immunotherapy resistance in TNBC
Immunotherapy Resistance in TNBC
TNBC accounts for approximately 15–20% of all breast cancer cases and is considered one of the most aggressive subtypes because of its high risk of recurrence and metastasis. In recent years, PD-1 or PD-L1 checkpoint inhibitors have provided new therapeutic opportunities. However, many patients still experience limited benefit or develop resistance shortly after treatment begins. Most previous studies investigating immunotherapy resistance have focused on tumor cells or immune cells themselves. However, researchers have increasingly begun to recognize that other components of the tumor microenvironment may play important roles in shaping therapeutic responses.
Sensory Nerves Drive Immune Exclusion
In this study, researchers analyzed 360 clinical samples of TNBC and reported that perineural invasion in tumor tissues was strongly associated with poor prognosis and a reduced response to immunotherapy. Further analysis revealed that the dominant nerve type infiltrating these tumors is sensory neurons, which normally transmit pain and touch signals. Tumors enriched with sensory nerves frequently exhibit an “immune-excluded” phenotype, in which immune cells accumulate around the tumor but fail to penetrate its core. This pattern suggested that sensory neurons might actively shape the immune landscape of the tumor microenvironment.
How Sensory Neurons Build a Stromal Barrier
To understand the mechanism underlying this phenomenon, researchers have conducted a series of mechanistic studies using neural-related animal models. They reported that tumor cells release signals that activate nearby sensory neurons. Once activated, these neurons stimulate cancer-associated fibroblasts to produce large amounts of collagen and other extracellular matrix components. As these materials accumulate, they form a dense stromal barrier that physically prevents immune cells from entering the tumor. “When sensory neurons become highly active, a dense matrix barrier gradually forms within the tumor,” explained Prof. Jiang, “This barrier effectively blocks immune cell infiltration and limits the effectiveness of immunotherapy.” When researchers inhibited sensory neuron signaling in animal models, the stromal barrier weakened, immune cells were able to infiltrate tumors more effectively, and tumor growth slowed.
Repurposing a Migraine Drug to Enhance Immunotherapy
Encouragingly, the researchers also identified a potential therapeutic strategy. In multiple animal models, suppressing sensory nerve signaling significantly improved the antitumor activity of immunotherapy when the two treatments were used together. The key compound used in the study was rimegepant, a CGRP receptor antagonist widely prescribed for migraine. Given that clinical safety data for this drug have already been established, repurposing it for cancer treatment could accelerate the path toward clinical translation. “This strategy of drug repurposing allows an existing clinical therapy to gain new applications in cancer treatment,” said Prof. Jiang, “It may help bring new treatment options to patients more quickly.”
A New Perspective from Cancer Neuroscience
Researchers believe that this study highlights the importance of considering the neuro–tumor–immune axis as an integrated system in cancer biology. “For a long time, the nervous system has been overlooked in cancer research,” said Prof. Shao. “Our findings suggest that targeting sensory neurons may provide a new way to overcome immunotherapy resistance and improve outcomes for patients with TNBC.”

